When choosing medical assistant teaching materials for hybrid or online programs, prioritize resources that cover all three accreditation domains (psychomotor, cognitive, and affective), include medical-grade equipment, provide guided protocols for independent practice, integrate with your LMS, support modular pricing for rolling admissions, and meet shipping demands at scale. Accredited MA programs need materials that work across modalities, document competency for CAAHEP or ABHES, and prepare students to perform confidently from day one at their externship site.
The medical assistant profession is on a tear right now. The U.S. Bureau of Labor Statistics projects 12 percent job growth from 2024 to 2034, with about 112,300 openings hitting the market every single year for the next decade. That’s four times faster than the national average for all occupations. Institutions are responding by building new MA programs or expanding existing ones, and a growing number of those programs are going online or hybrid to reach more students.
That expansion makes sense. General undergraduate certificate program enrollment is up 20 percent above 2020 levels. Enrollment in accelerated online allied health programs has climbed 15 percent in recent years. Students want flexible, career-focused pathways, and MA programs that deliver online or hybrid options are the ones capturing that demand.
But choosing medical assistant teaching materials for an online or hybrid program is a fundamentally different exercise than choosing materials for a traditional on-campus program. MAs don’t just learn content from a screen. These materials need to support students in a number of skills-based areas, some of which include:
- Drawing blood, administering injections, taking vital signs, running ECGs, and performing urinalysis
- Mastering billing codes, medical terminology, and patient scheduling workflows
- Developing professional communication skills, empathy, and ethical judgment
That’s a lot of ground to cover. The materials you choose will either make that possible or leave your students with gaps they’ll carry straight into their externships.
This article breaks down what program directors, clinical coordinators, and instructors should be evaluating when choosing medical assistant teaching materials for hybrid and online program delivery..
Medical Assistant Teaching Materials Need to Cover More than Content
Here’s something that catches a lot of programs off guard when they start shopping: most products on the market were designed to do one thing well, and only one thing. Textbooks and digital courseware handle the knowledge side. Supply vendors ship physical equipment. But accredited MA programs can’t operate in silos like that.
CAAHEP-accredited programs must document student achievement across 154 total competencies. ABHES-accredited programs have 44. Both accrediting bodies require evidence across three domains: psychomotor, cognitive, and affective. Graduates of programs accredited by either body are eligible to sit for the CMA (AAMA) certification exam, so the stakes for thorough competency coverage are high.
For anyone who hasn’t memorized accreditation jargon, here’s the quick breakdown:
- Psychomotor competencies are the hands-on clinical procedures: Drawing blood. Administering injections. Measuring blood pressure.
- Cognitive competencies cover knowledge-based areas like pharmacology, medical terminology, billing and coding, and EHR workflows.
- Affective competencies are the ones people tend to underestimate: professionalism, empathy, ethical judgment, patient communication.
What makes the MA role unique in allied health is that it blends clinical and administrative work. A nursing program can focus heavily on clinical skills because that’s the job. But an MA might be drawing blood at 9 a.m. and processing insurance claims at 10. That dual nature means medical assistant teaching materials need to be broader in scope than what most single-purpose products deliver.
A content publisher that covers billing codes beautifully but can’t teach a student how to perform a subcutaneous injection is only solving half the problem. A supply vendor that ships medical-grade syringes without any instructional framework is solving a different half. And the programs that struggle most are the ones trying to stitch together three or four different vendor relationships to cover all three domains. It works on paper, but it’s a headache and rarely works in practice.
The Real Challenge with Online and Hybrid Delivery
There’s a detail about online MA programs that trips up a surprising number of people, including some prospective students. Hybrid delivery has become prevalent for many online MA programs, and the 2026 guide to online medical assistant programs confirms it: legitimate programs pair virtual coursework with structured hands-on practice and a minimum 160-hour clinical externship.
The harder question sits upstream of that externship. Do students arrive ready to perform vitals, venipuncture, injections, and EKG setup, or does the preceptor spend the first week teaching what should already be muscle memory? Closing that readiness gap is where online and hybrid programs win or lose, and it demands a pre-clinical experience that drills core competencies before students step on site.
So when we talk about choosing medical assistant teaching materials for online programs, we’re really talking about materials that work across two modalities at the same time:
- The virtual component needs to handle knowledge acquisition, administrative skill building, and conceptual understanding of clinical procedures.
- The hands-on component needs to give students real-world practice with physical instruments, following actual clinical protocols.
Hands-on Skills Require Guided Practice
A 2025 scoping review examined how hybrid teaching develops competence in health sciences students. The findings confirmed what most educators already sense intuitively: online instruction works well for knowledge acquisition, but hands-on clinical skills require structured, guided practice. You can’t watch a video on phlebotomy and then walk into a clinical site ready to draw blood. The muscle memory, the procedural confidence, the feel of the equipment in your hands all come from repetition with the right tools.
This is also where faculty capacity enters the conversation. A lot of clinical coordinators are spending as many hours building their course content as they are teaching. Think about all the time that goes into:
- Uploading materials to the LMS and building course shells from scratch
- Creating assessment rubrics that map to specific competencies
- Sourcing supplies from one vendor and trying to match them to content from another
- Troubleshooting technical issues that eat into the first few weeks of every term
It’s a huge time sink, and it pulls faculty away from the work that matters most: mentoring students, evaluating competency, and building relationships with clinical partners.
Medical assistant teaching materials that arrive pre-built, with guided protocols already connected to the LMS, change that equation entirely. Instead of spending weeks on course setup, instructors are able to select skills labs aligned to their course and focused competencies at the start of their program.
What to Look for in Medical Assistant Teaching Materials for Hybrid and Online Programs
Not every product on the market is built for hybrid delivery, and the ones that claim to be aren’t always telling the full story. Here’s what separates medical assistant teaching materials that work for students and faculty from the ones that create more problems than they solve.
The Materials
Three-domain coverage in a single solution. This is the big one. If your materials only address psychomotor skills, you’re still on the hook for cognitive and affective content. If they only cover cognitive, your students aren’t getting hands-on practice. Look for materials that integrate all of the following:
- Clinical skills labs: phlebotomy, injections, vital signs, blood glucose testing, ECG, urinalysis
- Administrative and cognitive content: billing and coding, medical terminology, patient scheduling, prescription forms and labeling
- Affective learning: communication, professionalism, ethics
Buying separate products for each domain creates integration headaches, assessment gaps, and vendor management overhead that no program director needs.
Medical-grade equipment that mirrors real clinical settings. Students heading to externships need to practice with instruments they’ll encounter in physician offices and outpatient clinics. There’s a meaningful difference between practicing on consumer-grade simulation tools and working with the same equipment a clinical site uses daily. When students make that transition from training to externship, familiarity with the tools reduces anxiety and builds the kind of procedural confidence that clinical preceptors notice right away.
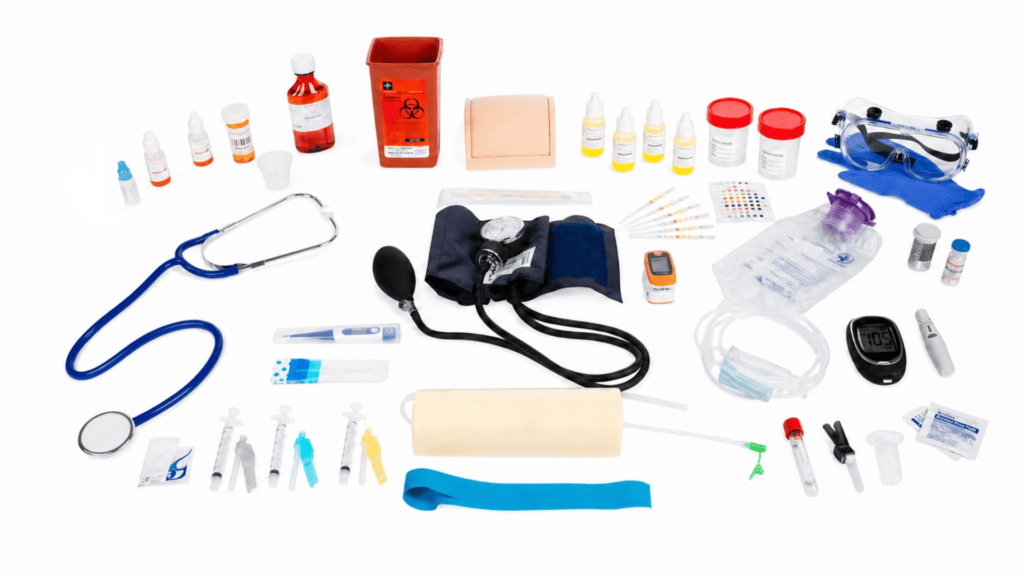
Guided protocols, not just a box of supplies. This distinction matters more than it might seem at first glance. Shipping physical materials without structured instruction puts the entire content development burden back on faculty. A good guided protocol does three things:
- Walks students through exact clinical techniques step by step
- Explains the rationale behind each action so students understand the “why,” not just the “how”
- Provides a framework for self-assessment so students can gauge their own progress
For distance learners who don’t have an instructor physically present during practice, this is the difference between meaningful skills practice and just expensive unboxing.
The Delivery
LMS integration and built-in assessment tools. Accreditation requires documented evidence of student competency. If your medical assistant teaching materials live outside your LMS, you’re asking faculty to track progress manually across separate systems. That eats hours and invites errors. Look for materials that:
- Connect directly to your LMS without requiring custom setup
- Include auto-grading and proctor tools
- Give instructors visibility into who’s on track and who’s falling behind
That data isn’t just helpful for accreditation visits. It lets faculty intervene early with students who need extra support, before a small gap becomes a big problem.
Modular and flexible packaging. This one’s especially important for programs with rolling admissions. Many MA programs, particularly at community colleges and career-focused institutions, enroll students throughout the year rather than in fixed cohorts. A student entering mid-cohort shouldn’t have to purchase a full semester of materials they won’t use.
Per-student, per-competency pricing models match cost to actual need. Modular structures also support remediation use cases, where an instructor assigns targeted practice in a specific skill area before externship and continuing education or bridge programs for career changers coming back into the medical field.
Shipping and scalability. Hybrid and online MA programs don’t ship to one campus loading dock. They ship to hundreds or thousands of individual student addresses, on a tight pre-term window, with no margin for error. Three signals separate vendors who can promise scale from vendors who have proven it.
- Ask the vendor to name programs they have supported through rapid enrollment growth
- Ask how many kits the vendor has shipped in a single pre-term window, and what their largest cohort looks like today.
- Push for the on-time rate and the process they follow when something goes wrong.
The Externship Readiness Test for Medical Assistant Teaching Materials
Every decision you make about medical assistant teaching materials eventually shows up in one place: the externship site. That’s where clinical preceptors aren’t shy about sharing feedback when students arrive unprepared.
Clinical sites don’t expect perfection. But they do expect a few things from day one:
- Familiarity with standard clinical equipment
- Understanding of basic clinical workflows and procedures
- The ability to communicate professionally with patients and staff
One MA program director, quoted in All Allied Health Schools, described communication and critical thinking as among the hardest skills to develop independently, noting that many younger students have limited prior work experience to draw from.
Materials that combine virtual learning with hands-on practice address this from both directions. The virtual component teaches the “why” behind each procedure: why we use a specific needle gauge for intramuscular injections, why blood glucose readings matter for patient care decisions, why infection prevention protocols exist. The hands-on component builds the muscle memory and procedural fluency that clinical sites expect. Students who’ve done both arrive at externships understanding what they’re doing and why, and that shows.
There’s a longer-term strategic angle here too. As clinical sites become more selective about which programs they accept students from (and this is a trend that’s picking up speed), the quality of your students’ preparation becomes a competitive differentiator for your program. Programs that consistently produce strong externs build better clinical partnerships. That means easier placements, better feedback loops, and a stronger reputation in the local healthcare community.
A Quick Word on Cost and Scalability
Budget conversations around medical assistant teaching materials can get complicated, partly because the price tag on the materials themselves is only one piece of the picture. Consider what programs are already spending on:
- Faculty hours building digital content and course shells
- Sourcing and assembling supplies independently
- Managing relationships with multiple vendors for different parts of the curriculum
- Tracking competency documentation manually across spreadsheets or disconnected systems
Those hidden costs add up fast, and they tend to scale poorly. A process that works for 20 students becomes a logistical headache for 200.
With individual Skill Packs, Standard and Customizable kits, there are many options that support different budgets. The right cost comparison isn’t “what does this product cost per student” in isolation. It’s “what does our current approach cost when we factor in faculty time, supply sourcing, vendor management, and documentation overhead, and how does that change as we grow.”
Scalability matters here. Primary care shortage areas grew 21 percent in just one year. The need for trained MAs isn’t waning. Programs that pick medical assistant teaching materials built for scale (consistent outcomes whether you have two sections or twelve) are the ones that can grow confidently without proportional increases in faculty workload.
Choosing Materials That Match Where MA Education Is Heading
The MA profession is moving fast. The scope of practice is widening as primary care physician shortages push more responsibilities to medical assistants. In fact, the AAMC projects a shortage of up to 86,000 physicians by 2036, which means MAs will be picking up tasks and responsibilities that would have seemed unlikely even five years ago. Programs that select medical assistant teaching materials based solely on today’s competency lists risk falling behind as the profession evolves.
Forward-thinking programs are looking for materials that check a few specific boxes:
- Cover all three competency domains in a single, integrated solution
- Work seamlessly across online and on-campus modalities
- Scale with enrollment growth without requiring proportional increases in faculty time
- Free up faculty to do the high-value work that no product can replace: mentoring students, evaluating clinical readiness, and maintaining strong relationships with externship partners
The programs that get this right won’t just pass their next accreditation review. They’ll build a reputation as the place that produces MAs who show up ready to work.
If you’re evaluating medical assistant teaching materials for your hybrid or online program, explore how Science Interactive’s complete MA skills lab integrates hands-on and virtual practice across all CAAHEP and ABHES competency domains, with guided protocols, medical-grade equipment, and LMS connectivity built in.
Frequently Asked Questions: Medical Assistant Teaching Materials
What are medical assistant teaching materials?
Medical assistant teaching materials include textbooks, digital courseware, hands-on lab kits, virtual simulations, and guided protocols used to train students in the clinical, administrative, and professional competencies required by CAAHEP and ABHES accreditation standards.
What should I look for in medical assistant teaching materials for online programs?
Look for materials that cover all three competency domains (psychomotor, cognitive, and affective), include medical-grade equipment for hands-on practice, provide guided protocols for independent learning, integrate with your LMS, offer flexible per-student pricing for rolling admissions, and meeting scalable shipping demands without error.
Do online MA programs require hands-on training materials?
Yes. Accredited online MA programs are hybrid models that require structured hands-on practice and a minimum 160-hour clinical externship. Fully online programs without hands-on components don’t qualify students for the CMA credential through the AAMA.
How many CAAHEP and ABHES competencies do MA programs need to cover?
CAAHEP-accredited MA programs must document student achievement across 154 total competencies spanning psychomotor, cognitive, and affective domains. ABHES-accredited programs require coverage of 44 competencies across the same three domains.
Discover more articles

How to Choose Medical Assistant Teaching Materials for Hybrid and Online Programs

You Don’t Have to Buy the Whole Kit: How Nursing Skill Packs Work

