Teaching clinical skills in an online MA program requires a hybrid approach: virtual instruction for cognitive foundations paired with guided, hands-on practice using medical-grade equipment. Programs that combine structured protocols, three-domain competency coverage, and built-in assessment produce students who arrive at externships ready to perform confidently from day one.
More than half of all U.S. postsecondary students now take at least one online course. IPEDS data shows that 54.3 percent of students are enrolled in some form of distance education, up from 37.2 percent in Fall 2019. Medical Assistant programs are riding that wave, and for good reason. Students want flexibility. Working adults, parents, and career changers need programs that meet them where they are, not programs that require them to show up on campus five days a week.
Here’s the challenge: clinical skills are physical. You can’t learn an intramuscular injection from a lecture recording. You can’t build phlebotomy confidence by watching someone else do it on video. Accrediting bodies know this. That’s why they require hands-on practice and a minimum 160-hour clinical externship.
So the question for program directors and instructors becomes how to teach clinical skills in a way that prepares students for the externship, the certification exam, and the job beyond both. This article walks through what the research says, what’s working in practice, and what to look for when building or refining your approach.
Teaching Clinical Skills Across 3 Domains, Not Just One
Teaching clinical skills in an online MA program means covering more ground than most people realize. CAAHEP requires documented competency across 154 standards. ABHES requires 44. Both span three distinct domains:
- Psychomotor competencies are the hands-on procedures: phlebotomy, injections, vital signs, ECG, blood glucose testing, urinalysis.
- Cognitive competencies cover knowledge areas like medical terminology, pharmacology, billing and coding, and EHR workflows.
- Affective competencies are the ones that tend to get overlooked, but can often set professionals apart: patient communication, professionalism, empathy, ethical judgment.
Most digital platforms handle the cognitive domain well: terminology quizzes, billing scenarios, pharmacology modules. That’s the stuff that translates naturally to a screen. Most supply kits handle the psychomotor, at least partially. They ship the equipment that lets students practice procedures.
But almost nobody addresses affective competencies in a systematic, assessable way. And when you’re teaching clinical skills online, the gaps between these domains get wider because there’s no physical lab environment where they naturally overlap.
Worth noting: the MA role is uniquely broad in allied health. A nursing program can focus heavily on clinical skills because that’s the core of the job. But an MA might draw blood at 9 a.m. and process insurance claims at 10. That dual clinical and administrative scope makes teaching clinical skills more complex than it is in a single-discipline program like phlebotomy or coding. The list of what counts as “clinical” is longer, and the variety of skills students need to demonstrate is wider.
What the Research Says About Teaching Clinical Skills at a Distance
The evidence on hybrid clinical skills instruction is clearer than you might expect, and it points in a consistent direction.
A study published in BMC Medical Education tested clinical skill retention in medical students 18 months after simulation-based training. The results were sobering:
- 55% of students were deficient in three or more skills
- A significant number had never practiced some skills after the initial teaching session
- Students who practiced more frequently performed better
- Skill decay happened across both psychomotor and cognitive domains
The researchers’ conclusion was straightforward: deliberate practice, under the guidance of an engaged instructor, is a key component of skill mastery.
That finding alone should make program directors think carefully about how they structure clinical skills practice for distance learners. A single lab session or a one-time video demonstration isn’t enough. Students need repeated, structured practice with the right equipment and clear guidance on technique.
Other recent research reinforces this:
- A 2025 experimental study found that combining flipped classroom instruction with practice significantly improved students’ self-assessed clinical abilities compared to traditional methods alone.
- A systematic review published in ScienceDirect concluded that active teaching methods in distance learning led to measurable improvements in clinical decision-making and student confidence.
- A scoping review in Simulation in Healthcare found that simulation-based learning before clinical placements increased student confidence, improved communication skills, and developed clinical reasoning.
The through-line across all of this research is consistent. Teaching clinical skills remotely works best when the practice is structured, guided, and repeated. Watching a demonstration once doesn’t build muscle memory. The research calls for “deliberate practice,” and it requires both the right tools and the right instructional framework.
The Most Effective Approach for Teaching Clinical Skills in Online MA Programs
The programs that are teaching clinical skills effectively in online and hybrid formats share a handful of common strategies. None of them are revolutionary on their own, but it’s the combination that makes them impactful.
Guided protocols that stand in for the instructor’s physical presence.
When a student is practicing a venipuncture technique at their kitchen table instead of in a campus lab, the instructional scaffolding has to be airtight. A good guided protocol does three things:
- Walks through exact clinical techniques step by step
- Explains the rationale behind each action so students understand the “why,” not just the mechanics
- Includes a self-assessment framework so students can check their own work before moving on
For asynchronous distance learners, this is what replaces the instructor looking over their shoulder. Shipping a box of supplies without this kind of structured guidance puts the entire content development burden back on faculty, and most clinical coordinators are already stretched thin.
Medical-grade equipment that students will actually see at clinical sites.
This sounds obvious, but it matters more than a lot of programs realize. There’s a meaningful difference between practicing with consumer-grade simulation tools and working with the same instruments a clinical site uses daily.
When students transition from training to their externship, familiarity with the equipment reduces anxiety and builds the kind of procedural confidence that clinical preceptors notice right away. Students who’ve never handled a real glucometer or a professional-grade stethoscope before their first day at a clinical site are starting from behind before they even walk in the door.

Assessment that documents competency, not just course completion.
Accreditation requires evidence that students have achieved specific competencies. A passing grade on a multiple-choice quiz doesn’t demonstrate that a student can perform a blood draw. Look for materials that:
- Focus on lessons and skills labs that are directly aligned with accreditation
- Offer LMS-integrated progress tracking so faculty can see who’s on track and who’s falling behind
- Give instructors early warning when a student needs extra support, before a small gap compounds into a serious problem heading into externship
Content that doesn’t require faculty to build it from scratch.
A lot of clinical coordinators are spending as many hours building their digital course content as they are teaching. Think about all the time that goes into:
- Creating course shells and uploading materials to the LMS
- Developing assessment rubrics mapped to specific competencies
- Sourcing supplies from one vendor and trying to align them with content from another
- Troubleshooting integration issues that chew up the first few weeks of every term
Teaching clinical skills well is hard enough. Building the entire digital infrastructure for it shouldn’t be on your clinical coordinator’s plate too. Materials that arrive pre-built, mapped to CAAHEP and ABHES competencies, and connected to your LMS give faculty their hours back for the work that only they can do: mentoring students, evaluating readiness, and maintaining relationships with clinical partners.
Modular structure for rolling admissions and remediation.
Plenty of MA programs, especially at community colleges and career-focused institutions, don’t operate on fixed semester schedules. Students enter throughout the year. A modular approach to teaching clinical skills lets students start at any point and work through specific competency areas independently rather than waiting for a new cohort.
It also supports pre-externship remediation, where an instructor identifies a specific skill gap and assigns targeted practice in that area. Flexible per-student, per-competency pricing structures make this financially workable for both the institution and the student. For a full breakdown of how to choose teaching materials for MA programs, check out this resource.
Where Teaching Clinical Skills Gets Tested: The Externship
Every approach to teaching clinical skills eventually gets graded in one place: the externship site. That’s where clinical preceptors see firsthand whether students are prepared or not.
Clinical sites don’t expect perfection from day one. But they do expect a few things:
- Baseline familiarity with standard clinical equipment
- Understanding of workflows, not just isolated procedures
- The ability to communicate professionally with patients and staff
Valley College’s MA Externship Handbook describes the evaluation process bluntly: instructors use an Externship Preparation Checklist and their professional judgment to determine whether a student is ready to begin. Once on site, preceptors evaluate students informally throughout the experience, and deficiencies are brought to the student’s attention as soon as they’re identified. This is a closely monitored process, not a passive observation period.
Programs that approach teaching clinical skills with both conceptual depth (the virtual component that builds understanding of “why”) and procedural repetition (the hands-on guided practice that builds muscle memory and confidence) consistently produce stronger externs. Students understand what they’re doing and can explain the reasoning behind it, which is a noticeably different posture than students who memorized steps from a textbook but never practiced them with real equipment.
There’s a strategic dimension too. Clinical sites are becoming more selective about which programs they accept students from. Programs that consistently send well-prepared externs build stronger clinical partnerships, meaning easier placements, better feedback loops, and a reputation that attracts both students and clinical partners over time.
Teaching Clinical Skills That Prepare Students for What’s Coming
The bar for teaching clinical skills in MA programs is only going to rise.
In the 2026 National Resident Matching Program, family medicine had the lowest fill rate of any specialty at 83.6%, leaving 899 positions unfilled. As primary care physician pipelines shrink, the healthcare system leans harder on medical assistants to pick up tasks and responsibilities that used to stay with other roles. The scope of what MAs are expected to do is expanding, and programs that teach clinical skills based only on today’s competency lists risk falling behind as the profession evolves.
Programs that invest in structured, evidence-based approaches for teaching clinical skills now, covering all three competency domains using both virtual and hands-on modalities, are the ones that will produce graduates who are ready for what the profession looks like in three years, not just today.
If you’re building or refining how your program approaches teaching clinical skills online, explore our MA skills lab for guided protocols, medical-grade equipment, and LMS-integrated assessment across CAAHEP and ABHES competency domains.
Frequently Asked Questions: Teaching Clinical Skills
How do you teach clinical skills in an online medical assistant program?
Accredited online MA programs use a hybrid model that pairs virtual instruction with structured, hands-on practice using medical-grade equipment and guided protocols. Students also complete at least 160 hours of clinical externship at a healthcare facility.
What clinical skills do medical assistant students need to learn?
MA students must develop psychomotor skills (phlebotomy, injections, vital signs, ECG, urinalysis), cognitive knowledge (medical terminology, billing, pharmacology), and affective competencies (patient communication, professionalism, ethics) to meet CAAHEP or ABHES accreditation standards.
Can you learn clinical skills online?
You can learn the cognitive foundations of clinical skills online, but accredited programs require hands-on practice with real equipment. Fully online programs without a hands-on component don’t qualify students for the CMA credential.Do clinical skills decay without practice? Yes. Research published in BMC Medical Education found that 55% of students were deficient in three or more clinical skills when re-tested 18 months after initial training. Teaching clinical skills through deliberate, repeated practice with guided feedback is essential for retention.
Discover more articles
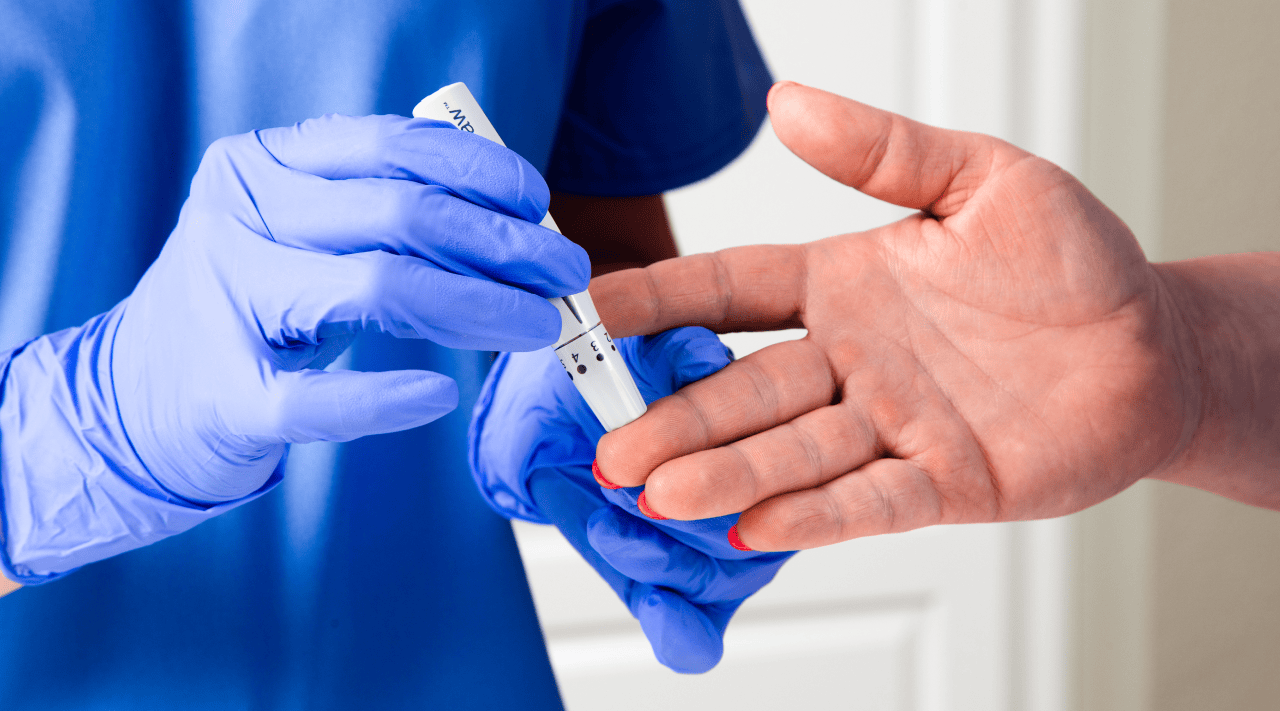
Teaching Clinical Skills in an Online Medical Assistant Program: Here’s What Works

How to Choose Medical Assistant Teaching Materials for Hybrid and Online Programs

