Becoming a medical assistant instructor after years of clinical practice is a bigger shift than most people expect. The clinical expertise translates, but the teaching infrastructure (the LMS, the curriculum mapping, the assessment documentation) is all new. These are the tips for MA instructors that they wish they had known before starting: strategies for navigating the clinician-to-educator transition, managing a skills lab, closing the feedback gap, and building student confidence across all three competency domains.
You’ve drawn blood thousands of times. You can take a full set of vitals in your sleep. You know how a real clinic runs because you’ve lived it.
None of that fully prepares you for teaching and cultivating those kinds of skills in 25 students who’ve never held a syringe.
MA programs are expanding fast to meet workforce demand. In fact, 85% of healthcare facilities report allied health staffing shortages, including medical assistants. That growth means programs need more instructors, and they’re recruiting from the clinical workforce. That’s smart, because clinical experience is irreplaceable.
But the transition from clinician to educator is well-documented as one of the hardest professional identity shifts in healthcare. That’s why we’re covering the things experienced MA instructors wish someone had told them before day one. Not the obvious stuff, but the practical, on-the-ground realities that’s often not covered in orientation.
The Clinician-to-Educator Shift is Real
You know how to do the work. Teaching someone else to do it is a completely different skill set.
A 2024 systematic review examining the transition from clinical practice to academia found a pattern that shows up over and over:
- Fear of failure in a role where you used to feel confident
- Battles with professional identity (you went from expert to novice overnight)
- Culture shock moving from a clinical environment to an academic one
- Feelings of being unprepared for curriculum design, assessment, and classroom management
The review noted that it can take up to three years to fully adopt a new professional identity as an educator. Three years. That’s a long time to feel like you’re finding your footing.
A 2025 review reinforced this, finding that clinicians moving into education face identity shifts, compensation tensions, and a lack of structured onboarding. Support systems are crucial for making the transition work, but they’re often lacking.
Researchers describe one of the core challenges as “difficulty extracting tacit knowledge.” In plain terms: the stuff you do automatically after years of clinical practice is the hardest stuff to explain to someone who’s never done it. You don’t think about how you position your hand during a venipuncture. You just do it. Breaking that down into teachable steps requires a different kind of thinking than performing the procedure yourself.
The good news: your clinical credibility is your biggest asset as an MA instructor. Students connect with real-world stories and firsthand experience more than they connect with textbook explanations. The instructor who shares field stories, throws curveball questions from real patient encounters, and tells students “here’s what the textbook says, and here’s what can happen” is the one students remember and learn from.
The Feedback Gap: What Students Need
If there’s one thing that comes up consistently when MA students talk about their programs, it’s feedback.
The pattern students describe looks like this:
- The instructor demonstrates a procedure
- Students practice on their own
- Students are tested
The problem is step two. Faculty are overburdened by workload and technology barriers for online skills labs, that they can’t always provide timely feedback at scale. Students want formative evaluation before summative testing. They want to know whether they’re doing it right while they’re still learning, not after the grade is already in the book.
When graded work comes back weeks later, the feedback loses most of its value. A correction on a quiz from two months ago doesn’t help a student who’s already moved on to new material.
The research backs this up. A study published in BMC Medical Education found that:
- 55% of students were deficient in three or more clinical skills when retested 18 months later.
- Students who practiced more frequently and received supervision retained more.
- Skill decay happened across both psychomotor and cognitive domains.
The researchers concluded that deliberate practice with engaged supervision is essential for skill mastery. One-and-done demonstrations don’t stick.
What this means for a new MA instructor:
- Build in practice checkpoints before assessments. If students can self-assess along the way using structured protocols, they catch their own mistakes before those mistakes get graded. Guided protocols with built-in self-check frameworks do this systematically rather than relying on an instructor being available for every student at every moment.
- Speed up the feedback loop. Features in your LMS like auto-grading and proctor tools reduce the turnaround time on competency checks. If your materials require you to manually grade every single skill evaluation, you’ll fall behind. One instructor grading 25 students across dozens of competencies can’t keep up without some automation.
- Use assessment data to intervene early. When progress tracking is integrated into the LMS, you can see which students are falling behind before it becomes a crisis. That early warning is the difference between a student who gets extra help in week four and a student who fails their externship in week twelve.
Teaching Across Three Domains
Most new MA instructors feel confident teaching clinical procedures. That’s what they know. The harder part is everything else.
CAAHEP requires documented competency across 154 standards. ABHES requires 44. Both span three domains:
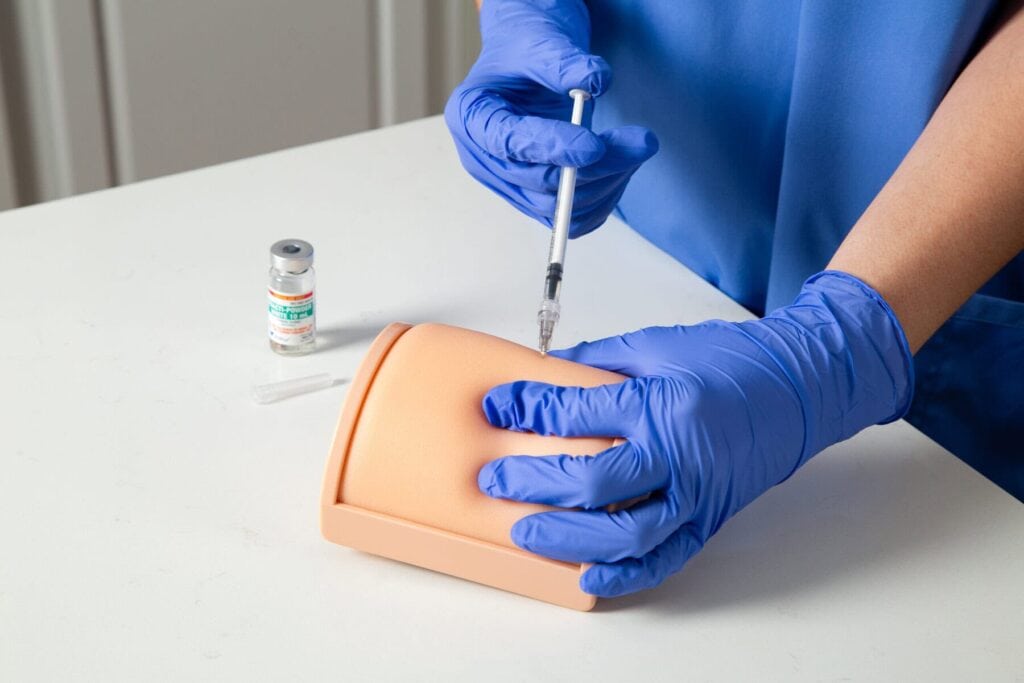
- Psychomotor: the hands-on clinical procedures. Phlebotomy, injections, vital signs, ECG, blood glucose testing, urinalysis. This is where most MA instructors feel at home.
- Cognitive: medical terminology, pharmacology, billing and coding, EHR workflows. This is where students often struggle with retention. The lab skills click faster than the book learning for many students, which is the opposite of what a lot of programs assume.
- Affective: patient communication, professionalism, empathy, ethical judgment. This domain often gets taught informally, if it gets taught at all. But it matters enormously in clinical settings, and students notice when it’s missing from their training.
The challenge for a new MA instructor is that most available materials only cover one or two of these domains well. A content publisher handles cognitive. A supply vendor handles psychomotor. Nobody seems to systematically address the affective.
Materials that arrive pre-built, with guided protocols and cognitive content already mapped to accreditation standards, remove the curriculum development burden from a new MA instructor who’s already learning to teach. That matters, because building a three-domain curriculum from scratch while simultaneously figuring out how to manage a classroom is a fast track to burnout.
Running a Skills Lab as a New MA Instructor
Running a skills lab is one of the steepest learning curves for a new MA instructor. In clinic, you supervised one person at a time. In a lab, you’ve got 15 to 25 students all practicing simultaneously, and every one of them needs your attention.
A few things that help:
Improve competency focus areas with skills lab partners. Practicing clinical skills with skills lab partners allows students to communicate with different personalities, explain procedures to each other, and adapt to different working styles. That’s part of the affective domain in action, built right into the skills lab without needing a separate lesson on communication.
Use guided protocols to scale your attention. When students have structured, step-by-step procedural guides with self-assessment frameworks, they can practice independently while you circulate and provide targeted feedback where it’s needed most. You can’t be everywhere at once. Good protocols extend your presence for students.
Use equipment that mirrors clinical settings. Students who practice with medical-grade instruments build procedural confidence faster. When your students walk into their externship and recognize the equipment, their anxiety drops. Clinical preceptors notice that confidence immediately.
Plan for hybrid and online delivery. For programs where students practice at a distance, the skills lab challenge gets even bigger. The guided protocol has to do the heavy lifting that an MA instructor would normally do in person. That’s why protocol design matters so much: it has to include not just the steps, but the rationale, the common mistakes, and the self-check framework.
NHA notes that digital platforms with real-time performance insights allow instructors to identify individual student needs and remediate weaknesses before they progress too far. That kind of visibility is especially valuable for a new MA instructor who’s still developing their instinct for spotting struggling students.
What Experienced MA Instructors Would Tell Their Day-One Selves
A few things that don’t show up in any job description but come up consistently from instructors who’ve been through the first-year learning curve.
Your clinical stories are your superpower. Use them constantly. Students connect with “here’s what happened when I was working in a cardiology office” more than they connect with “turn to chapter seven.” Real-world context makes content stick in ways that straight lecture can’t replicate. For more on maximizing teaching impact and student engagement in hybrid labs, check out this resource.
You don’t have to build everything from scratch. Pre-built, competency-mapped content saves hundreds of hours. Spending your first semester creating course shells, writing rubrics, sourcing supplies, and troubleshooting LMS integrations from zero is a recipe for burnout. Materials that arrive ready to assign, mapped to CAAHEP and ABHES standards, and already connected to your LMS give you your hours back for actual teaching. Here’s a full breakdown of how to choose medical assistant teaching materials.
Get comfortable with the LMS before the semester starts. Technical troubleshooting in front of students erodes confidence, both yours and theirs. Spend time with the platform before day one. If your materials plug in without requiring custom setup, that’s one less thing on your plate.
Build relationships with externship site preceptors early. Their feedback on what students need to show up ready to perform is the single best curriculum input you’ll get. Those relationships also become the pipeline for placing your students, which matters more as clinical sites get pickier about which programs they partner with.
Active learning beats straight lecture for knowledge retention. Review games, flash cards, case-based scenarios, partner practice with verbal or video walkthroughs. Students who struggle with the cognitive domain often can do better when the information is delivered through interaction rather than reading. Not every new MA instructor figures this out on their own, and nobody tells you in orientation.
Setting New MA Instructors Up to Succeed
The transition from clinician to MA instructor is one of the most rewarding moves in healthcare education. It’s also one of the least supported.
Programs that set their instructors up with the right tools (pre-built content, integrated assessment, guided protocols that scale one-on-one teaching to a full lab) don’t just retain better faculty. They produce better-prepared students.
And in a market where the majority of healthcare facilities are short on allied health staff, producing well-prepared MA graduates isn’t just an academic goal. It’s a workforce imperative.
If these tips for MA instructors were helpful, explore our MA skills lab for guided protocols, medical-grade equipment, and LMS-integrated assessment across CAAHEP and ABHES competency domains.
Frequently Asked Questions: Tips for MA Instructors
What qualifications do you need to be an MA instructor?
Most programs require a current or recent CMA, RMA, or equivalent credential, several years of clinical experience in both front and back office, and often an associate or bachelor’s degree. Some institutions also require teaching experience or a teaching credential.
What’s the hardest part of being a new MA instructor?
Research consistently identifies the clinician-to-educator transition as a major challenge. New instructors must learn curriculum design, LMS management, assessment documentation, and classroom management while simultaneously teaching clinical and administrative skills across three competency domains.
How can new MA instructors improve student skill retention?
Structure frequent, guided practice with real equipment and build in formative assessment before summative evaluations. Research shows that deliberate, repeated practice with feedback is essential for clinical skill retention.
Discover more articles
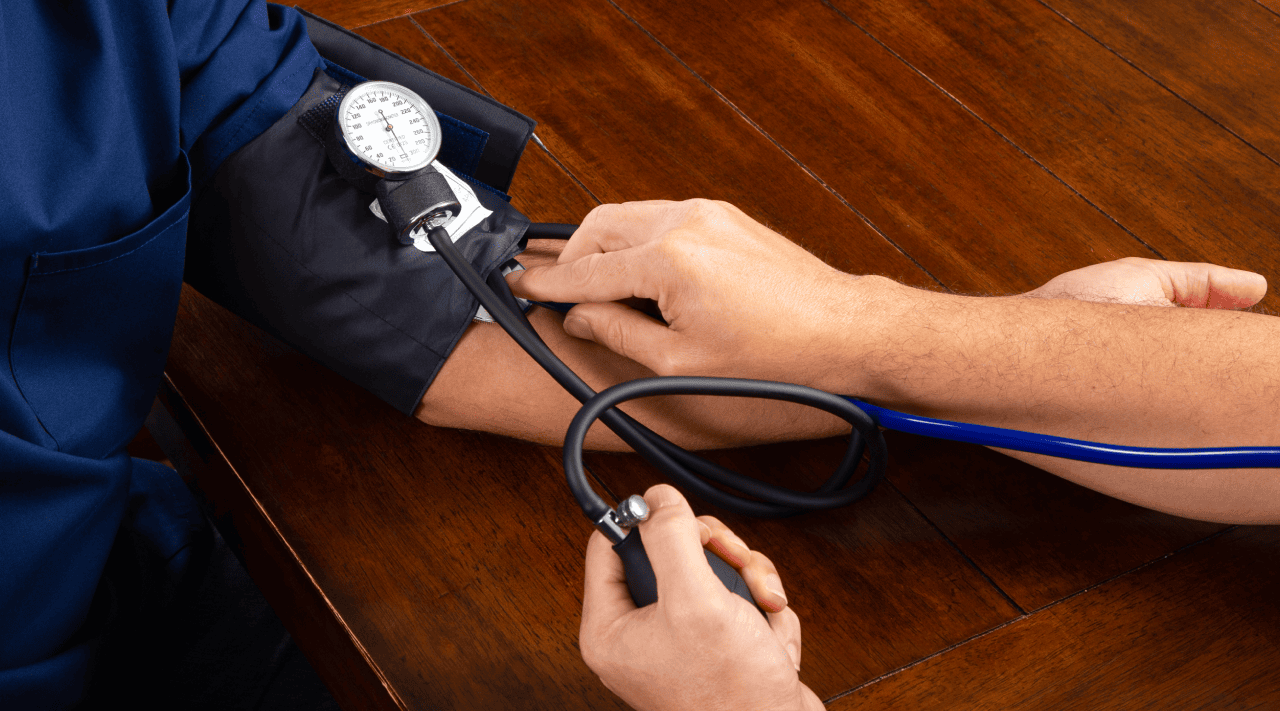
What New MA Instructors Wish They’d Known Before Their First Semester
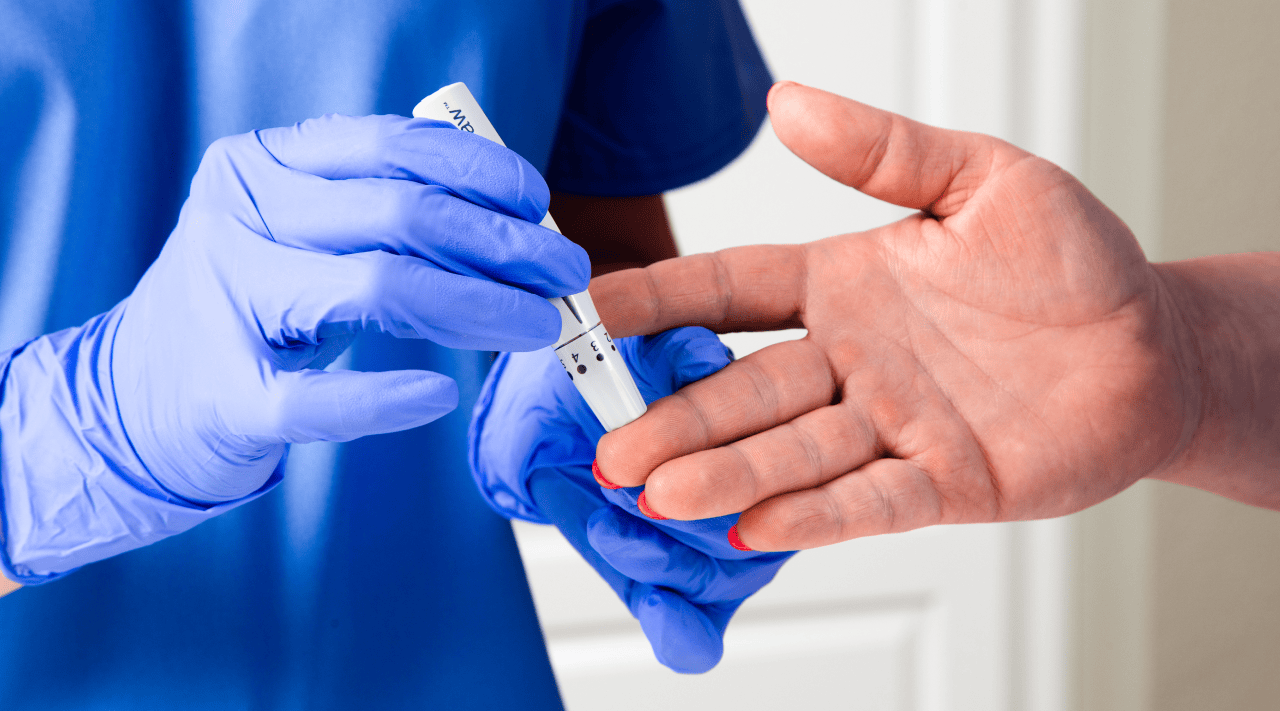
Teaching Clinical Skills in an Online Medical Assistant Program: Here’s What Works

